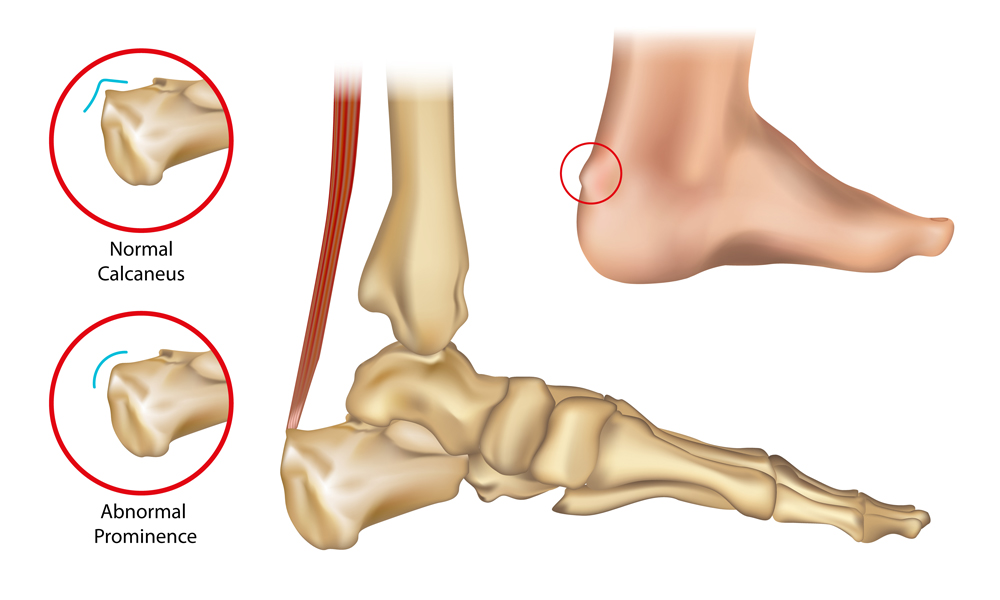
Causes of Haglund's Deformity
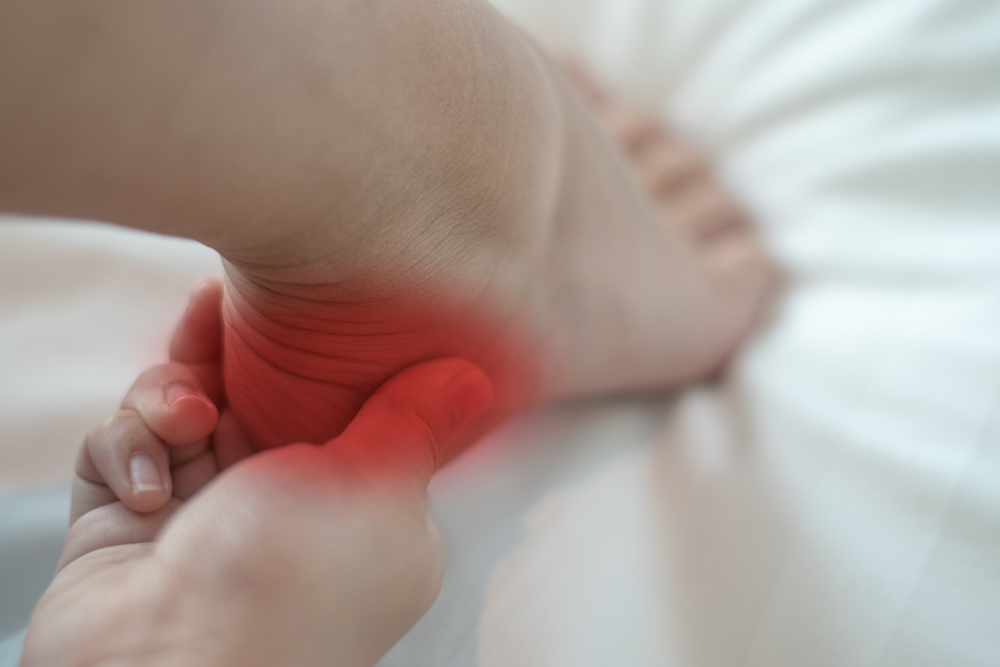
Symptoms
Apart from enlarged bone growth, Haglund’s can cause blisters on the heels. The back can become tender, inflamed, and red. In cases where the pain is present, it tends to increase after rest when the person starts walking again. There can be swelling and limping.
Any examination should consider a history of arthritis, gout, or another rheumatologic condition.
Tight Achilles Tendon
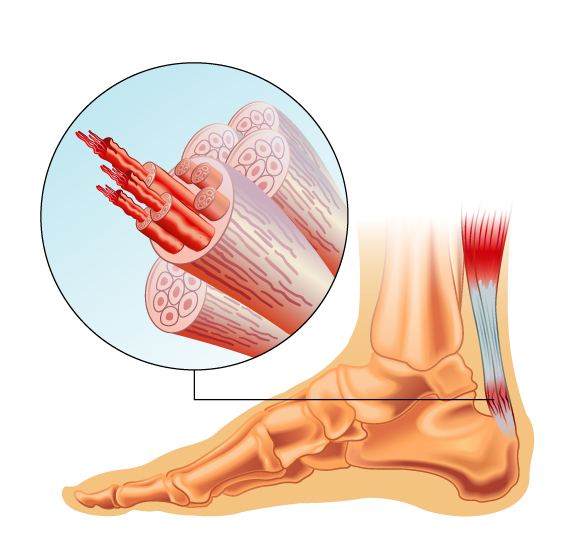
This section is devoted to the most common cause of Haglund’s deformity. Overuse of the Achilles tendon results in tendinitis, chronic inflammation of the tissue band that connects the heel bone to the calf muscles.
Athletes, especially runners, are most commonly affected by Achilles tendinitis. It’s particularly frequent in people who suddenly increase the duration or intensity of training.
If left untreated, Achilles tendinitis might give way to Haglund’s deformity. Otherwise, it can be treated at home with relative ease. A doctor’s supervision and self-care tend to be enough to prevent it from reoccurring.
In more severe cases, the tendon can break, which will necessitate surgical intervention.
Typically, the first symptom of Achilles tendinitis is a slight ache above the heel or in the back of the leg. Sprinting, climbing stairs, or extended physical activity precedes instances of more severe pain.
Risk Factors
- Male sex - it affects men more often
- Achilles tendinitis is more common with age
- A naturally flat foot arch puts more pressure on the tendon
- Running in worn-out shoes
- Running uphill
- Cold weather
- Obesity
- Tight calf muscles
- Medical conditions
People who have high blood pressure or psoriasis face a higher risk of developing the condition.
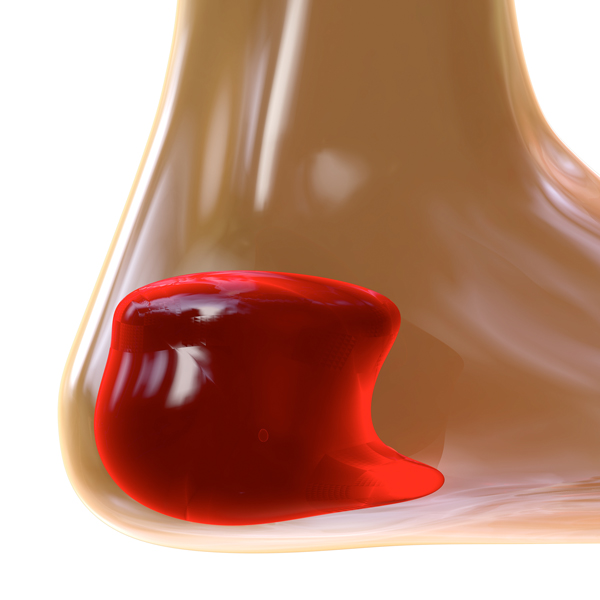
Diagnosis of Haglund's Deformity
Radiographs of the ankle from the side and clinical evaluation usually suffice to diagnose the condition. The diagnosis is often based on clinical findings and history, though.Particularly in the early stages, the radiographic criteria to diagnose Haglund’s lesion are not clear-cut. Plain radiographs can feature some typical angles.
In difficult cases, your doctor might order a magnetic resonance imaging (MRI) exam. It will show a calcaneal spur pressing on the Achilles tendon. This might go alongside synovial pooling and thickening in the retrocalcaneal bursa with high signal and density in the tendon’s insertional fibers. Sometimes, your exam findings will include swelling in the adjoining adipose tissue pad behind the Achilles tendon.
Treatment of Haglund's Deformity
There are numerous ways to treat Haglund’s deformity. These include immobilization, changing the heel height in footwear, non-steroid anti-inflammatory drugs (NSAIDs), local steroid injections, physiotherapy, and more.
If the area is badly inflamed, a soft cast or walking boot can be used to immobilize it. The inflammation is expected to go away on its own.
Your doctor might prescribe custom-made orthotics to change the position of the foot. This is expected to help reduce the friction caused by the shoes.
It is advisable to wear shoes without a rigid back. The enlarged bone requires footwear with a wider heel counter to be accommodated properly.
Insoles for Haglund's Deformity
Adding insoles can help alleviate the symptoms of Haglund’s deformity. If you can’t wear shoes with an open back, they can help keep your feet comfortable and reduce the pressure on your heels. The good news is that there are all kinds of insoles on the market now. There are insoles for skates, snow sports, running shoes, casual shoes, official shoes, hiking boots, and high heels, among others.
Additional Benefits of Insoles
Insoles can also help with lower back pain, whether due to Haglund’s deformity or another cause. Anyone with some kind of foot imbalance or dysfunction is prone to develop back pain. Ankle or foot problems can cause imbalances or lower back misalignment. Those will exacerbate back pain with time.
This is where custom-made insoles come in. They are inserted into the shoe to remedy irregular or abnormal posture while walking by realigning the ankle. An orthopedic doctor can prescribe insoles to reduce back pain, heel pain, foot pain, or all three.

Like shoes, insoles will get worn out with time and need to be replaced once every few years.
Other Conditions Caused by Mechanical Foot Problems
Common foot problems that can result in abnormal or irregular gait or posture include:
- Foot numbness
- Nerve pain
- Neuroma
- Tarsal tunnel syndrome
- Plantar fasciitis, resulting in chronic arch or heel pain
- Bunions
- Bunionettes
- Excessive foot supination or pronation (rolling out/in)

Insoles Let Soft Tissue Heal
If your insoles help improve your gait and posture, this will improve the condition of the soft tissue in the lower back, reducing pain. In theory, any ankle or foot problem leading to compromised gait or posture can cause pain in the lower back. Potentially, it can also cause pain in the ankles, knees, hips, or other weight-bearing joints.
Back pain is not always present in people with ankle or foot problems, of course. In cases where it is, treating the ankle or foot syndrome can potentially reduce back pain.
Foot insoles have no adverse side effects and are frequently inexpensive, making them a go-to option for Haglund’s deformity or joint or back problems in general. They are comfortable and easy to use. They do take some getting used to, but you’ll be able to go about your daily routine in no time. They are also a drug-free, non-invasive, and safe treatment approach for anyone who wishes to cut down on or completely avoid taking pain medication.
Stopping the Domino Effect from Occurring
Another common issue with this kind of foot problem is the so-called domino effect. What do we mean? Let’s take someone with a normal foot arch as an example. If you drew a line along the shin bone to the foot, it would go between their big toe and their second toe. If you drew this same line through a foot with an excessively high or a flat arch, which has caused ankle and foot pronation (rolling inward), it would shift, passing through the big toe.
People whose ankles and feet are pronated shift their body weight to the outside of their feet, which causes pain, bunions, and more.
By wearing insoles that realign the back of the foot to keep this body-weight shift from occurring, you can prevent the domino effect.
Surgery for Haglund's Deformity
In very few cases, the condition will require surgery. As is the case for many conditions, surgery is the last resort. It is performed under general or local anesthesia. The orthopedic surgeon makes an incision to the side of the Achilles tendon, extending from 3–4 cm proximally to the superior calcaneus tuberosity to 2–3 cm distally. The surgeon identifies the tendon by blunt and sharp dissection. They place a right-angle retractor between the tendon and the superior and posterior calcaneal tuberosity borders.
The superior border and the retrocalcaneal bursa are now exposed without moving any part of the Achilles tendon away from the calcaneus. The surgeon might have to raise a small portion of the tendon to resect the bone adequately. First, they remove the retrocalcaneal bursa. Then, they use an osteotome to remove the superior part of the tuberosity. This resection becomes easier after placing a few drill holes in the chosen osteotomy site.
The surgeon removes any calcification. They then apply a short, well-padded, non-weight-bearing cast. It is removed around three weeks after the intervention. The sutures are removed one week prior.
The patient then starts plantar flexion exercises and wears a weight-bearing cast boot. High-heeled shoes will not be comfortable at that point or perhaps at any point thereafter. In some cases, all discomfort goes away after six months, and you can wear such shoes again.
Potential Complications
The vast majority of surgeries to eradicate Haglund’s deformity is successful. In very rare cases, one of the following complications may arise:
- Constant pain at the back of the heel
- Achilles tendon avulsion
- Ankle stiffness
- Wound breakdown
- Nerve injuries
- Incisional neuroma

Final Thoughts
Haglund’s deformity is one of the most common causes of pain at the back of the heel in adults. In most cases, conservative treatment is effective. Surgery is rarely resorted to, if ever.
Want to discuss Haglund’s deformity with a specialist? Fill out the form below or call us for a consultation.
